Normal Immune Response
The pathogen enters the body and encounters macrophages, these macrophage cells then engulf the pathogen via phagocytosis. Once phagocytosed fragments of the pathogen’s antigens are displayed on the macrophages cell surface. Macrophages displaying antigens on their cell surface are known as antigen presenting cells (APC’s)
T-Helper cells specific to the antigen displayed by the APC recognises and interacts with the APC. This interaction causes the release of interleukin-1 molecules from the APC, in turn this causes the T-Helper cell to release Interleukin-2 and express interleukin-2 receptors on its cell surface. Interleukin-2 causes growth and proliferation of cytotoxic T-cells, it also causes proliferation of B-cells, as well as increased production of the immunoglobulins made by B-cells.
From here the immune response follows two paths, one mediated by cytotoxic T-cells and the toher mediated by B-cells.
Cytotoxic T-Cell Route:
Infected cells display antigens on their cell surfaces, cyctotoxic T-cells which are specific to this antigen bind to the infected cell and produce the chemicals perforin, granulysin, and granzymes.
- Perforin and granulysin cause pores to form in the infected cell’s plasma membrane.
- Granzymes may then enter the cell, activating proteases which then go on to trigger apoptosis.
The death of the infected cell also results in the death of the invading pathogen within it, so stopping further spread of infection to other cells.
B-Cell route:
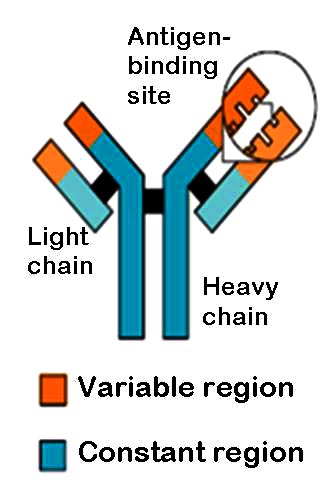 B-cells, like T-cells come in millions of different varieties, each recognising a different antigen.
B-cells, like T-cells come in millions of different varieties, each recognising a different antigen.
When a B-cell is activated by its corresponding T-Helper cell it differentiates into a plasma cell. Plasma cells are able to produce vast quantities (100’s-1000’s per second per cell) of antibodies specific to the invading organism.
These antibodies are released into the bloodstream where they bind to any corresponding antigens they encounter on the surface of pathogens. This marks these pathogens for ingestion by macrophages and helps to recruit natural killer cells.
Other B-cells do not, when activated, differentiate to become plasma cells, they instead become memory B-cells. These memory cells can persist for years or for an entire lifetime.
On secondary invasion by the same pathogen they allow the immune response to be much faster and efficient, sometimes resolving the infection before symptoms have even occurred. This immunonlogical memory is what gives us immunity to a disease once we have had it ie chickenpox, or once we have been immunised against it ie polio.
References
Picture courtesy of Wikimedia Commons
Diagram courtesy of Wikiemdia Commons
Human physiology:from cells to systems, Lauralee Sherwood, Cengage Learning, 2008
Immunology: an illustrated outline, David K. Male, Elsevier Health Sciences, 2004
